Determining how the pattern of bone healing affects the strain of plate implant via frequency detection: A biomechanical cadaveric study
Keywords:
Acoustic, bone healing, frequency, pattern, plate, strain, unionAbstract
Background: Detecting bone union is crucial in treating bone fractures to prevent complications, including implant failure and bone nonunion. To date, there are numerous methods and new innovative devices for detecting bone union via strain measurements, such as strain gauges, fluid level displacement, contrast media, and frequency changes. Moreover, there is a trend toward increasing these methods in the future. However, the patterns of bone healing studied with these methods do not provide a standard for determining the true bone healing process.
Objective: This study aimed to identify the most appropriate bone healing pattern for detecting bone healing using strain measurements via frequency changes.
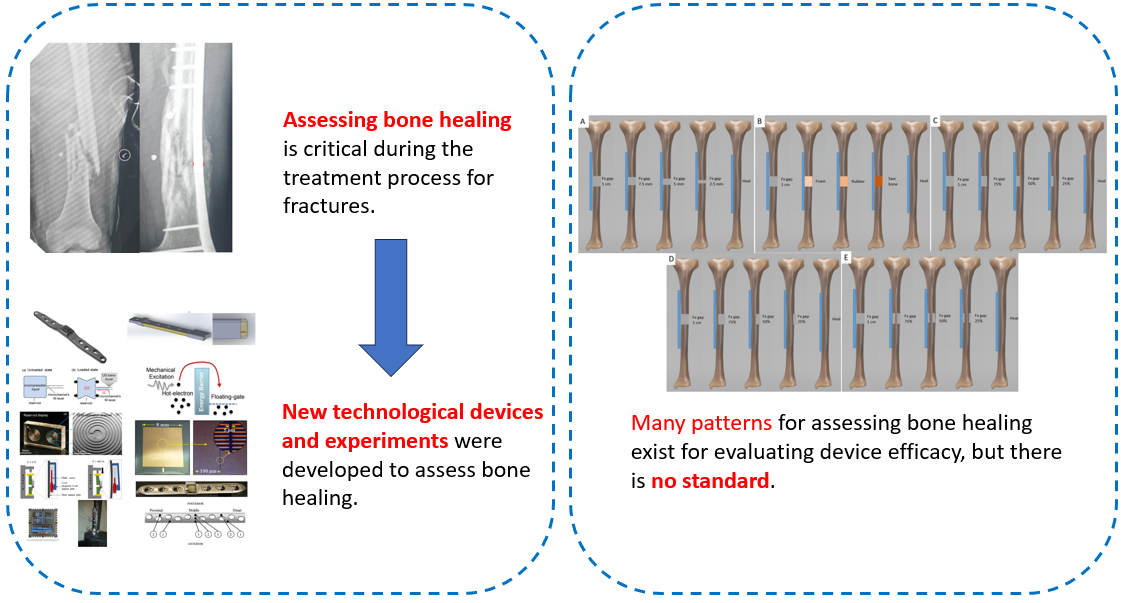
Methods: Twenty cadaveric tibial bones were tested for five different bone healing patterns, including fractures with gap distances, material replacements, and healing from the outer side, inner side, and middle. Each healing pattern included four cadaveric bones evaluated under various axial loads of 100, 200, 300, and 400 N using an Instron ElectroPuls® E10000. Bone healing assessment employed bone union detection using a wire’s natural frequency plate to detect the strain change via frequency change.
Results: All bone healing patterns could evaluate bone union by comparing the frequency changes under axial loads of 100 and 400 N, with a mean difference of 32.4–39.8%. Only the fracture with gap distance and material replacement could be assessed gradually in each phase of healing (12.3% in gap of 2.5 mm, P < 0.01; 22.4% in gap of 5 mm, P = 0.04; 31.8% in gap of 7.5 mm, P = 0.005; 39.2% in gap of 10 mm, P = 0.004; and 11.0% in saw bone, P = 0.006; 19.5% in rubber, P < 0.001; 25.8% in foam, P < 0.001; 32.4% in fracture, P < 0.001).
Conclusions: The pattern of bone healing influences the assessment of bone union via the detection of strain changes. The methods involving gap distance and material replacement are the most suitable representation of normal bone healing.
Downloads
References
Zhu Z, Zhang T, Shen Y, Shan PF. The burden of fracture in China from 1990 to 2019. Arch Osteoporos 2023;19:1.
https://doi.org/10.1007/s11657-023-01353-4
Nyrhi L, Kuitunen I, Ponkilainen V, Huttunen TT, Mattila VM. Incidence of fracture hospitalization and surgery during pregnancy in Finland-1998-2017: a retrospective register-based cohort study. Arch Orthop Trauma Surg 2023;143:5719-25.
https://doi.org/10.1007/s00402-023-04931-w
GBD 2019 Fracture Collaborator. Global, regional, and national burden of bone fractures in 204 countries and territories, 1990-2019: a systematic analysis from the Global Burden of Disease Study 2019. Lancet Healthy Longev 2021;2:e580-e92.
Wu CY, Lee HS, Tsai CF, Hsu YH, Yang HY. Secular trends in the incidence of fracture hospitalization between 2000 and 2015 among the middle-aged and elderly persons in Taiwan: A nationwide register-based cohort study. Bone 2022;154:116250.
https://doi.org/10.1016/j.bone.2021.116250
Baertl S, Alt V, Rupp M. Surgical enhancement of fracture healing - operative vs. nonoperative treatment. Injury 2021;52 Suppl 2:S12-S7.
https://doi.org/10.1016/j.injury.2020.11.049
Nicholson JA, Makaram N, Simpson A, Keating JF. Fracture nonunion in long bones: a literature review of risk factors and surgical management. Injury. 2021;52 Suppl 2:S3-S11.
https://doi.org/10.1016/j.injury.2020.11.029
Siverino C, Metsemakers WJ, Sutter R, Della Bella E, Morgenstern M, Barcik J, et al. Clinical management and innovation in fracture non-union. Expert Opin Biol Ther 2024;24:973-91.
https://doi.org/10.1080/14712598.2024.2391491
Nicholson JA, Yapp LZ, Keating JF, Simpson A. Monitoring of fracture healing. Update on current and future imaging modalities to predict union. Injury 2021;52 Suppl 2:S29-S34.
https://doi.org/10.1016/j.injury.2020.08.016
Cunningham BP, Brazina S, Morshed S, Miclau T 3rd. Fracture healing: A review of clinical, imaging and laboratory diagnostic options. Injury 2017;48 Suppl 1:S69-S75.
https://doi.org/10.1016/j.injury.2017.04.020
Craig JG, Jacobson JA, Moed BR. Ultrasound of fracture and bone healing. Radiol Clin North Am 1999;37:737-51, ix.
https://doi.org/10.1016/S0033-8389(05)70126-3
Willems A, Iҫli C, Waarsing JH, Bierma-Zeinstra SMA, Meuffels DE. Bone union assessment with computed tomography (ct) and statistical associations with mechanical or histological testing: a systematic review of animal studies. Calcif Tissue Int 2022;110:147-61.
https://doi.org/10.1007/s00223-021-00904-6
Schwarzenberg P, Darwiche S, Yoon RS, Dailey HL. Imaging modalities to assess fracture healing. Curr Osteoporos Rep 2020;18:169-79.
https://doi.org/10.1007/s11914-020-00584-5
Haffner-Luntzer M, Müller-Graf F, Matthys R, Hägele Y, Fischer V, Jonas R, et al. Evaluation of high-resolution in vivo MRI for longitudinal analysis of endochondral fracture healing in mice. PLoS One 2017;12:e0174283.
https://doi.org/10.1371/journal.pone.0174283
Crönlein M, Rauscher I, Beer AJ, Schwaiger M, Schäffeler C, Beirer M, et al. Visualization of stress fractures of the foot using PET-MRI: a feasibility study. Eur J Med Res 2015;20:99.
https://doi.org/10.1186/s40001-015-0193-6
Sollini M, Trenti N, Malagoli E, Catalano M, Di Mento L, Kirienko A, et al. [18F]FDG PET/CT in non-union: improving the diagnostic performances by using both PET and CT criteria. Eur J Nucl Med Mol Imaging 2019; 46:1605-15.
https://doi.org/10.1007/s00259-019-04336-1
Windolf M, Varjas V, Gehweiler D, Schwyn R, Arens D, Constant C, et al. Continuous implant load monitoring to assess bone healing status-evidence from animal testing. Medicina (Kaunas) 2022;58:858.
https://doi.org/10.3390/medicina58070858
McGilvray KC, Unal E, Troyer KL, Santoni BG, Palmer RH, Easley JT, et al. Implantable microelectromechanical sensors for diagnostic monitoring and post-surgical prediction of bone fracture healing. J Orthop Res 2015;33:1439-46.
https://doi.org/10.1002/jor.22918
Najafzadeh A, Serandi Gunawardena D, Liu Z, Tran T, Tam HY, Fu J, et al. Application of fibre bragg grating sensors in strain monitoring and fracture recovery of human femur bone. Bioengineering (Basel) 2020;7:98.
https://doi.org/10.3390/bioengineering7030098
Borchani W, Aono K, Lajnef N, Chakrabartty S. Monitoring of postoperative bone healing using smart trauma-fixation device with integrated self-powered piezo-floating-gate sensors. IEEE Trans Biomed Eng 2016;63:1463-72.
https://doi.org/10.1109/TBME.2015.2496237
Kienast B, Kowald B, Seide K, Aljudaibi M, Faschingbauer M, Juergens C, et al. An electronically instrumented internal fixator for the assessment of bone healing. Bone Joint Res 2016;5:191-7.
https://doi.org/10.1302/2046-3758.55.2000611
Pelham H, Benza D, Millhouse PW, Carrington N, Arifuzzaman M, Behrend CJ, et al. Implantable strain sensor to monitor fracture healing with standard radiography. Sci Rep 2017;7:1489.
https://doi.org/10.1038/s41598-017-01009-7
Rajamanthrilage A, Arifuzzaman M, Millhouse P, Pace T, Behrend C, DesJardins J, et al. Measuring orthopedic plate strain to track bone healing using a fluidic sensor read via plain radiography. IEEE Trans Biomed Eng 2022;69:278-85.
https://doi.org/10.1109/TBME.2021.3092291
Umbrecht F, Wägli P, Dechand S, Gattiker F, Neuenschwander J, Sennhauser U, et al. Wireless implantable passive strain sensor: design, fabrication and characterization. J Micromech Microeng 2010;20:085005.
https://doi.org/10.1088/0960-1317/20/8/085005
Ledet EH, Caparaso SM, Stout M, Cole KP, Liddle B, Cady NC, et al. Smart fracture plate for quantifying fracture healing: preliminary efficacy in a biomechanical model. J Orthop Res 2022;40:2414-20.
https://doi.org/10.1002/jor.25254
Chancharoen P, Tangpornprasert P, Amarase C, Tantavisut S, Virulsri C. Design of osteosynthesis plate for detecting bone union using wire natural frequency.Sci Rep 2024;14:12569.
https://doi.org/10.1038/s41598-024-63530-w
Leong PL, Morgan EF. Measurement of fracture callus material properties via nanoindentation. Acta Biomater 2008;4:1569-75.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Chulalongkorn Medical Journal

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.









