Artificial intelligence decision support in automated breast ultrasound: improving diagnostic accuracy and reducing unnecessary biopsies
Keywords:
Artificial intelligence, breast neoplasms, ultrasoundAbstract
Background: The emerging roles of artificial intelligence (AI) support in the imaging of the breast have led to improved radiologist performance.
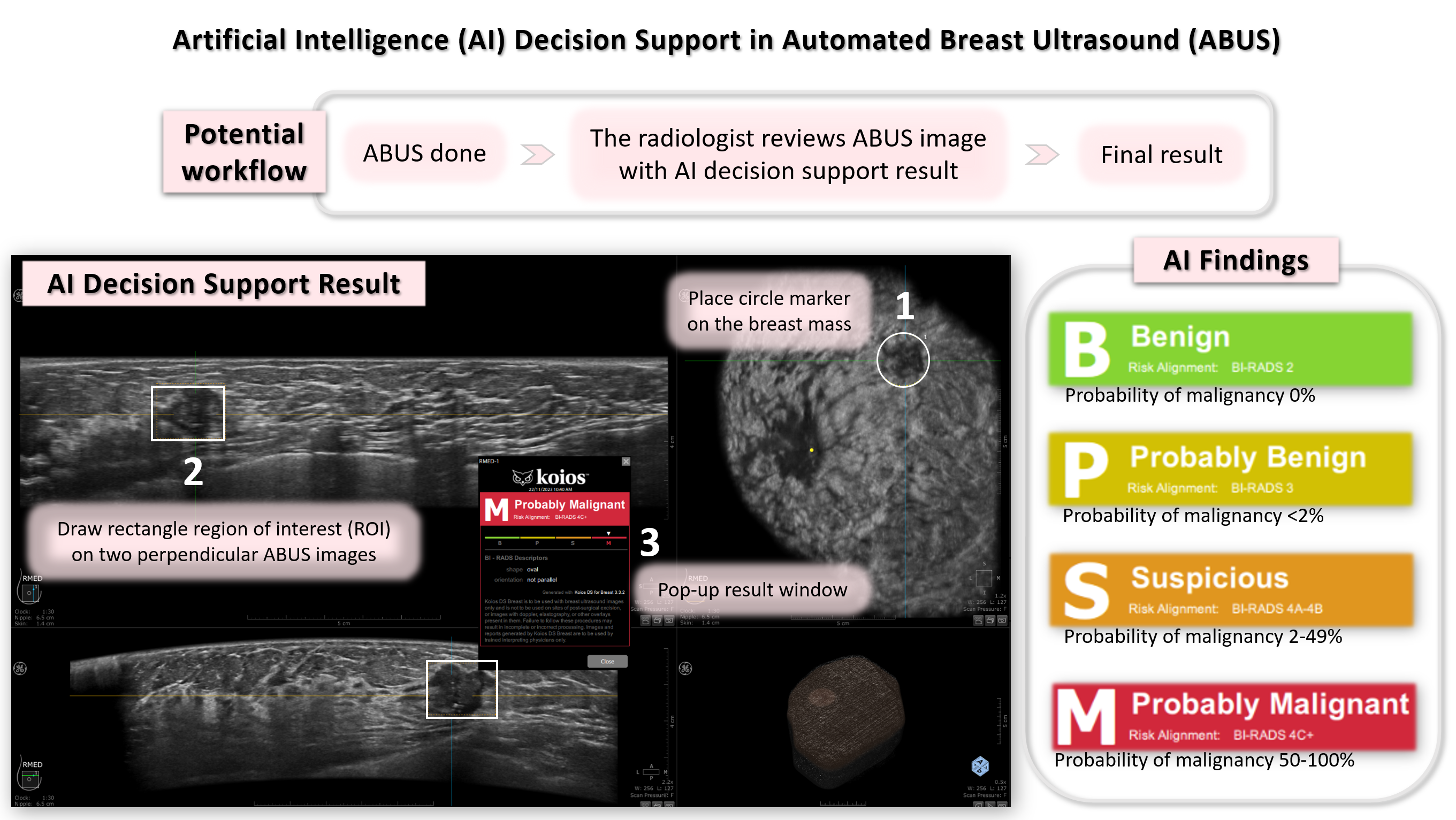
Objective: This study assessed the diagnostic performance of the AI decision support in the evaluation of breast masses using automated breast ultrasound (ABUS).
Methods: One hundred eighty-two patients (415 breast masses) who received ABUS were included. Two readers, including an experienced breast radiologist (reader 1) and the breast imaging fellow (reader 2), separately reviewed the ABUS images and the AI decision support according to the American College of Radiology BI-RADS 5th edition guidelines.
Results: In the 415 masses that were evaluated, 395 (95.2%) were benign, and 20 (4.8%) were malignant. The area under the receiver operating curve (AUC) of the AI decision support was 0.74 (95% confidence interval Original article (CI) 0.72–0.77) with a sensitivity and specificity of 100.0% and 48.6%, respectively. The integration of AI decision support significantly increased the AUC for both readers, from 0.82 (95% CI 0.74–0.91) to 0.85 (95% CI 0.76–0.93) for reader 1 (P < 0.001) and from 0.79 (95% CI 0.71–0.88) to 0.81 (95% CI 0.73–0.89) for reader 2 (P < 0.001). Furthermore, the AI decision support led to a 14.2% and 16.9% alteration in BI-RADS, with a 22.2% and 10.7% reduction in biopsies of benign masses for reader 1 and reader 2, respectively.
Conclusion: AI decision support demonstrates diagnostic performance comparable to that of radiologists, exhibiting high sensitivity and a high negative predictive value. Integrating AI into the diagnostic workflow may potentially enhance the diagnostic performance of radiologists across various experience levels and thereby contribute to a reduction in unnecessary biopsies of benign masses.
Downloads
References
Bray F, Laversanne M, Sung H, Ferlay J, Siegel RL, Soerjomataram I, et al. Global cancer statistics 2022:GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 2024;74:229-63.
https://doi.org/10.3322/caac.21834
Mainiero MB, Lourenco A, Mahoney MC, Newell MS, Bailey L, Barke LD, et al. ACR Appropriateness Criteria® breast cancer screening. J Am Coll Radiol 2016;13:R45-R49.
https://doi.org/10.1016/j.jacr.2016.09.021
Berg WA, Bandos AI, Mendelson EB, Lehrer D, Jong RA, Pisano ED. Ultrasound as the primary screening test for breast cancer: analysis from ACRIN 6666. J Natl Cancer Inst 2015;108:djv367.
https://doi.org/10.1093/jnci/djv367
Brem RF, Tabár L, Duffy SW, Inciardi MF, Guingrich JA, Hashimoto BE, et al. Assessing improvement in detection of breast cancer with three-dimensional automated breast ultrasound in women with dense breast tissue: the SomoInsight Study. Radiology 2015;274:663-73.
https://doi.org/10.1148/radiol.14132832
Mango VL, Sun M, Wynn RT, Ha R. Should we ignore, follow, or biopsy? Impact of artificial intelligence decision support on breast ultrasound lesion assessment. AJR Am J Roentgenol 2020;214:1445-52.
https://doi.org/10.2214/AJR.19.21872
Barinov L, Jairaj A, Becker M, Seymour S, Lee E, Schram A, et al. Impact of data presentation on physician performance utilizing artificial intelligence-based computer-aided diagnosis and decision support systems. J Digit Imaging 2019;32:408-16.
https://doi.org/10.1007/s10278-018-0132-5
Berg WA, López Aldrete AL, Jairaj A, Ledesma Parea JC, García CY, McClennan RC, et al. Toward AIsupported US triage of women with palpable breast lumps in a low-resource setting. Radiology 2023;307: e223351.
https://doi.org/10.1148/radiol.223351
Browne JL, Pascual MÁ, Perez J, Salazar S, Valero B, Rodriguez I, et al. AI: can it make a difference to the predictive value of ultrasound breast biopsy? Diagnostics (Basel) 2023;13:811.
https://doi.org/10.3390/diagnostics13040811
D'Orsi CJ, Sickles EA, Mendelson EB, Morris EA. ACR BI-RADS® atlas : breast imaging reporting and data system. Reston, VA: American College of Radiology; 2013.
Shoukri MM, Asyali MH, Donner A. Sample size requirements for the design of reliability studies: review and new results. Stat Methods Med Res 2004;13:251-71.
https://doi.org/10.1191/0962280204sm365ra
Berg WA, Gur D, Bandos AI, Nair B, Gizienski TA, Tyma CS, et al. Impact of original and artificially improved artificial intelligence-based computer-aided diagnosis on breast US interpretation. J Breast Imaging 2021;3:301-11.
https://doi.org/10.1093/jbi/wbab013
Lyu SY, Zhang Y, Zhang MW, Zhang BS, Gao LB, Bai LT, Wang J. Diagnostic value of artificial intelligence automatic detection systems for breast BI-RADS 4 nodules. World J Clin Cases 2022;10:518-27.
https://doi.org/10.12998/wjcc.v10.i2.518
Wang X, Meng S. Diagnostic accuracy of S-Detect for breast cancer on ultrasonography: a meta-analysis (PRISMA). Medicine (Baltimore) 2022;101:e30359.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Chulalongkorn Medical Journal

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.









