Performance and cost comparison of a rapid diagnostic test for malaria and microscopy: A cross-sectional diagnostic study in Gusau, Nigeria
Keywords:
Cost, microscopy, performance, rapid diagnostic tests, resource-limitedAbstract
Background: The shift from traditional microscopy to rapid diagnostic tests (RDTs) for malaria diagnosis is gaining popularity, especially in resource-limited settings where electricity supply is unstable and expertise is limited. However, trust issues arise from inconsistent performance across different RDT kits.
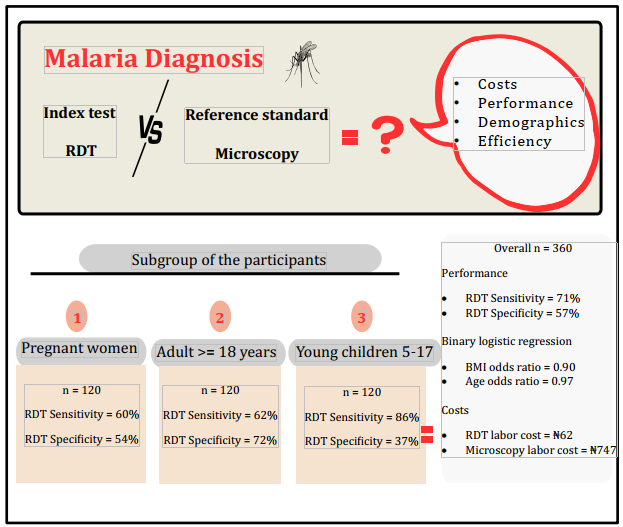
Objectives: This study aimed to identify variations in the performance and cost of an RDT brand for malaria among different population demographics, including pregnant women, young children, and adults, compared with microscopy as a gold standard.
Methods: The research was conducted in northwestern Nigeria and involved 360 participants who were stratified into three groups: children (5–17 years), adults (≥ 18 years), and pregnant women. Samples were examined using RDT and microscopy, and cost data were gathered from retrospective study expenses.
Results: The RDT exhibited higher sensitivity (86.1%) and a positive predictive value of 87.9% in children, but lower sensitivity (59.5%) and specificity (54.3%) in pregnant women. Logistic regression analysis indicated that the likelihood of testing positive decreased by 2.0% for each year of age (P = 0.046) and by 10.0% for each unit increase in body mass index (BMI) (P < 0.001) and was twice that of positivity in those who experienced vomiting (P = 0.004). Moreover, RDT had lower labor costs (₦61) than microscopy (₦746), which requires higher technical expertise.
Conclusion: RDTs offer a rapid diagnostic option for malaria, which may be suitable in resource-constrained settings for certain populations, such as children or adults. However, their limitations in pregnant women and the impact of age and BMI on accuracy necessitate supplementary tests where resources permit.
Downloads
References
Venkatesan P. Egypt declared malaria free. Lancet Microbe 2025;6:101052.
https://doi.org/10.1016/j.lanmic.2024.101052
Batte A, Namazzi R, Conroy AL. Acute kidney injury in severe malaria: a new dawn. Semin Nephrol 2025:45:151613.
https://doi.org/10.1016/j.semnephrol.2025.151613
Thellier M, Gemegah AAJ, Tantaoui I. Global fight against malaria: goals and achievements 1900-2022. J Clin Med 2024;13:5680.
https://doi.org/10.3390/jcm13195680
Liu Q, Jing W, Kang L, Liu J, Liu M. Trends of the global, regional and national incidence of malaria in 204 countries from 1990 to 2019 and implications for malaria prevention. J Travel Med 2021;28:taab046.
https://doi.org/10.1093/jtm/taab046
Shekarau E, Uzoanya M, Ogbulafor N. Severe malaria intervention status in Nigeria: workshop meeting report. Malar J 2024;23:177.
https://doi.org/10.1186/s12936-024-05001-1
Mezieobi KC, Alum EU, Ugwu OP, Uti DE, Alum BN, Egba SI, et al. Economic burden of malaria on developing countries: A mini review. Parasite Epidemiol Control 2025;30:e00435.
https://doi.org/10.1016/j.parepi.2025.e00435
Li J, Docile HJ, Fisher D, Pronyuk K, Zhao L. Current status of malaria control and elimination in Africa: epidemiology, diagnosis, treatment, progress and challenges. J Epidemiol Glob Health 2024;14:561-79.
https://doi.org/10.1007/s44197-024-00228-2
Lawal L, Buhari AO, Jaji TA, Alatare AS, Adeyemo AO, Olumoh AO, et al. Lingering challenges in malaria elimination efforts in sub Saharan Africa: Insights andpotential solutions. Health Sci Rep 2024;7:e2122.
https://doi.org/10.1002/hsr2.2122
Aribodor DN, Ugwuanyi IK, Aribodor OB. Challenges to achieving malaria elimination in Nigeria. Am J Public Health Res 2016;4:38-41.
Alghamdi JM, Al-Qahtani AA, Alhamlan FS, AlQahtani AA. Recent advances in the treatment of malaria. Pharmaceutics 2024;16:1416.
https://doi.org/10.3390/pharmaceutics16111416
Duffy PE, Gorres JP, Healy SA, Fried M. Malaria vaccines: a new era of prevention and control. Nat Rev Microbiol 2024;24:756-72.
https://doi.org/10.1038/s41579-024-01065-7
Li J, Saidi AM, Seydel K, Lillehoj PB. Rapid diagnosis and prognosis of malaria infection using a microfluidic point-of-care immunoassay. Biosens Bioelectron 2024;250:116091.
https://doi.org/10.1016/j.bios.2024.116091
Mbanefo A, Kumar N. Evaluation of malaria diagnostic methods as a key for successful control and elimination programs. Trop Med Infect Dis 2020;5:102.
https://doi.org/10.3390/tropicalmed5020102
Nyenke CU. Emerging techniques in malaria diagnosis. In: Sreenivasan A, Deepa K, Chtitambare K, Khan I, editors. Issues on health science. India: ZenToks Publ; 2024. p. 1-16
Wardhani P, Butarbutar TV, Adiatmaja CO, Betaub AM, Hamidah N. Performance comparison of two malaria rapid diagnostic test with real time polymerase chain reaction and gold standard of microscopy detection method. Infect Dis Rep 2020;12 Suppl 1:8731.
https://doi.org/10.4081/idr.2020.8731
Otambo WO, Olumeh JO, Ochwedo KO, Magomere EO, Debrah I, Ouma C, et al. Health care provider practices in diagnosis and treatment of malaria in rural communities in Kisumu County, Kenya. Malar J 2022; 21:129.
https://doi.org/10.1186/s12936-022-04156-z
Garba BI, Muhammad AS, Musa A, Edem B, Yusuf I, Bello NK, et al. Diagnosis of malaria: A comparison between microscopy and rapid diagnostic test among under-five children at Gusau, Nigeria. Sub Saharan Afr J Med 2016;3:96-101.
https://doi.org/10.4103/2384-5147.184371
Du YQ, Ling XX, Jin JJ, Zhou HY, Zhu S, Zhu GD, et al.Cost-effectiveness analysis of malaria rapid diagnostic test in the elimination setting. Infect Dis Poverty 2020;9:135.
https://doi.org/10.1186/s40249-020-00745-9
Almaw A, Yimer M, Alemu M, Belay H, Alebachew M, Abeje G, et al. Prevalence of clinical malaria and associated symptoms in pregnant women at Hamusit health center, Northwest Ethiopia. Heliyon 2024;10: e34240.
https://doi.org/10.1016/j.heliyon.2024.e34240
Maqsood A, Farid MS, Khan MH, Grzegorzek M. Deep malaria parasite detection in thin blood smear microscopic images. Appl Sci 2021;11:2284.
https://doi.org/10.3390/app11052284
Abdullahi K, Shinkafi S, Aguh B, Bilbis L, Danladi A, Mohammad B, et al. View of Malaria prevalence in Gusau Township, Nigeria (A preliminary report). Int J Sci for Glob Sustain 2020;6:88-93.
https://doi.org/10.57233/ijsgs.v6i1.135
Ajakaye OG, Ibukunoluwa MR. Performance evaluation of a popular malaria RDT in Nigeria compared with microscopy. J Parasit Dis 2020;44:122-5.
https://doi.org/10.1007/s12639-019-01170-y
Bisoffi Z, Sirima SB, Menten J, Pattaro C, Angheben A, Gobbi F, et al. Accuracy of a rapid diagnostic test on the diagnosis of malaria infection and of malariaattributable fever during low and high transmission season in Burkina Faso. Malar J 2010;9:192.
https://doi.org/10.1186/1475-2875-9-192
Chua CLL, Hasang W, Rogerson SJ, Teo A. Poor birth outcomes in malaria in pregnancy: recent insights into mechanisms and prevention approaches. Front Immunol 2021;12:621382.
https://doi.org/10.3389/fimmu.2021.621382
Martiáñez-Vendrell X, Skjefte M, Sikka R, Gupta H. Factors affecting the performance of HRP2-based malaria rapid diagnostic tests. Trop Med Infect Dis 2022;7:265.
https://doi.org/10.3390/tropicalmed7100265
Bosco AB, Nankabirwa JI, Yeka A, Nsobya S, Gresty K, Anderson K, et al. Limitations of rapid diagnostic tests in malaria surveys in areas with varied transmission intensity in Uganda 2017-2019: Implications for selection and use of HRP2 RDTs. PloS One 2020;15:e0244457.
https://doi.org/10.1371/journal.pone.0244457
Rogier E, Battle N, Bakari C, Seth MD, Nace D, Herman C, et al. Plasmodium falciparum pfhrp2 and pfhrp3 gene deletions among patients enrolled at 100 health facilities throughout Tanzania: February to July 2021. Sci Rep 2024;14:8158.
https://doi.org/10.1038/s41598-024-58455-3
Nadakou NT, Paraïso MN, Yobo JB, Makoutode CP, Sodjinou J, Tapha O, et al. Risk factors associated with malaria infection in children aged from 6 to 59 months in Niger: a cross-sectional study. BMC Public Health 2025;25:1001.
https://doi.org/10.1186/s12889-025-22211-7
Wilairatana P, Tangpukdee N, Krudsood S, Wilairat N, Wilairat P, Thebpatipat P. Overweight and obesity as protective factors in severe falciparum malaria. Southeast Asian J Trop Med Public Health 2019;50: 421-7.
Babayo S. Population bulge and food security in Nigeria: a positive or negative nexus. IJSSC 2023;1: 94-103.
https://doi.org/10.38142/ijssc.v1i3.91
Ojo AA, Maxwell K, Oresanya O, Adaji J, Hamade P, Tibenderana JK, et al. Health systems readiness and quality of inpatient malaria case-management in Kano State, Nigeria. Malar J 2020;19:384.
https://doi.org/10.1186/s12936-020-03449-5
Manoel PZ, Uwishema O, Manoel AZ, Dike IC, Yassin N, Mshaymesh S. Exploring the burden of noncommunicable diseases on surgical services in Africa: a comprehensive literature review. Ann Med Surg (Lond) 2025;87:2847-54.
https://doi.org/10.1097/MS9.0000000000003236
Bashar JM, Hadiza S, Ugochi OJ, Muhammad LS, Olufemi A, Eberechi U, et al. Charting the path to the implementation of universal health coverage policy in Nigeria through the lens of Delphi methodology. BMC Health Serv Res 2025;25:45.
https://doi.org/10.1186/s12913-024-12201-7
Chijioke MI, Olisah RC. Oil revenue and poverty in Nigeria: the south-south perspective in post covid-19 era. JEAR 2023;8:240-50.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Chulalongkorn Medical Journal

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.









