Factors influencing outcomes in neonatal abdominal surgery: surgeons’ perspectives
Keywords:
Neonatal abdominal surgery, neonatal mortality, risk factors, surgical complicationsAbstract
Background: Neonatal abdominal surgery is often indicated by congenital conditions, which present considerable morbidity and mortality risks. However, comprehensive surgical data and identification of complication-related risk factors are still lacking.
Objective: The objectives of this study were to characterize neonatal patients undergoing abdominal surgery and to identify prognostic factors associated with complications and mortality.
Methods: A retrospective study was conducted on newborn patients aged 0–30 days who underwent index surgery at a university hospital from 2013 to 2021. Categorical data were compared between the with and without complications groups. Complications were defined as any events that required intervention, either surgical or medical.
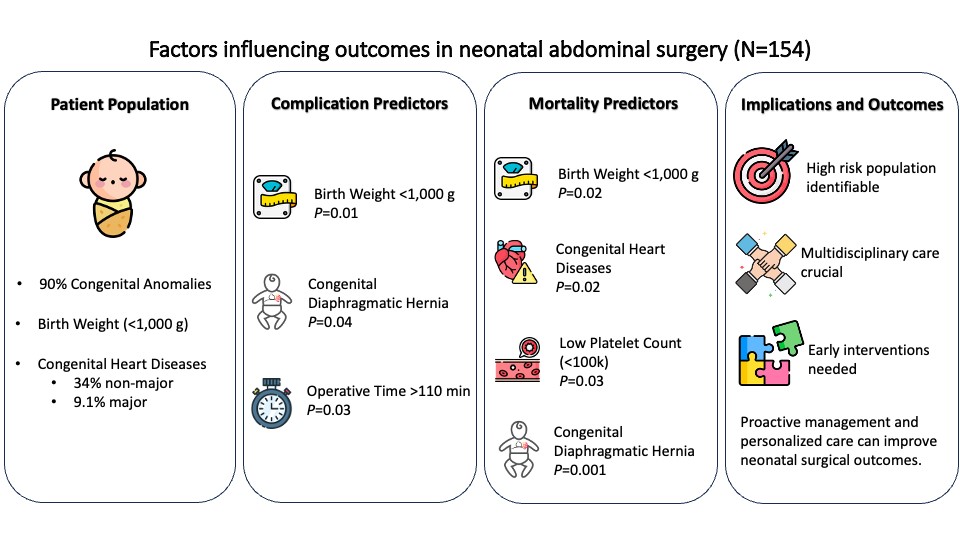
Results: There were 154 neonates undergoing 173 index procedures, and 19 patients had more than one condition. The five most common conditions requiring abdominal surgery included abdominal wall defect (31.0%), colorectal disease (16.0%), intestinal atresia (14.0%), necrotizing enterocolitis (8.0%), and meconium peritonitis (7.0%). The incidence of patients with at least one complication was 44.8%, and the mortality rate was 7.8%. Using logistic regression, factors associated with complications included birth weight <1,000 g (P = 0.01), APGAR (CDH) (P = 0.04), and operative time >110 min (P = 0.03). Significant influences on mortality were birth weight <1000 g (P = 0.02), cardiovascular anomalies (P = 0.02), CDH (P = 0.001), and platelet count <100,000/µL (P = 0.03).
Conclusion: This study provides valuable insights into factors that influence outcomes in neonatal abdominal surgery. Birth weight <1000 g, CDH, and operative time >110 min were identified as significant contributors to complications. Furthermore, birth weight < 1000 g, cardiovascular anomalies, CDH, and platelet count <100,000/µL strongly influence mortality. These findings emphasize the complexity of neonatal abdominal surgery with various conditions. Understanding these prognostic factors can help predict the outcome of neonatal abdominal surgery, and improving these outcomes may be achievable in the future.
Downloads
References
Hasan MS, Islam N, Mitul AR. Neonatal surgical morbidity and mortality at a single tertiary center in a low- and middle-income country: a retrospective study of clinical outcomes. Front Surg 2022;9:817528.
https://doi.org/10.3389/fsurg.2022.817528
Ugwu RO, Okoro PE. Pattern, outcome and challenges of neonatal surgical cases in a tertiary teaching hospital. Afr J Paediatr Surg 2013;10:226-30.
https://doi.org/10.4103/0189-6725.120886
Lissauer T. Thinking beyond global neonatal mortality rates. Paediatr Int Child Health 2015;35:171 3.
https://doi.org/10.1179/2046904715Z.000000000278
Bardi F, Bergman JEH, Bouman K, Erwich JJ, Duin LK, Walle HEK, et al. Effect of prenatal screening on trends in perinatal mortality associated with congenital anomalies before and after the introduction of prenatal screening: A population-based study in the Northern Netherlands. Paediatr Perinat Epidemiol 2021;35:654-63.
https://doi.org/10.1111/ppe.12792
Heino A, Morris JK, Garne E, Baldacci S, Barisic I, Cavero-Carbonell C, et al. The association of prenatal diagnoses with mortality and long-term morbidity in children with specific isolated congenital anomalies: A European register-based cohort study. Matern Child Health J 2024;28:1020 30.
https://doi.org/10.1007/s10995-024-03911-9
Bucher BT, Duggan EM, Grubb PH, France DJ, Lally KP, Blakely ML. Does the American College of Surgeons National Surgical Quality Improvement Program pediatric provide actionable quality improvement data for surgical neonates? J Pediatr Surg 2016;51:1440-4.
https://doi.org/10.1016/j.jpedsurg.2016.02.084
Siyotula T, Arnold M. An analysis of neonatal mortality following gastro-intestinal and/or abdominal surgery in a tertiary hospital in South Africa. Pediatr Surg Int 2022;38:721-9.
https://doi.org/10.1007/s00383-022-05100-7
Catre D, Lopes MF, Madrigal A, Oliveiros B, Viana JS, Cabrita AS. Early mortality after neonatal surgery: analysis of risk factors in an optimized health care system for the surgical newborn. Rev Bras Epidemiol 2013;16:943-52.
https://doi.org/10.1590/S1415-790X2013000400014
Catré D, Lopes MF, Madrigal A, Oliveiros B, Cabrita AS, Viana JS, et al. Predictors of major postoperative complications in neonatal surgery. Rev Col Bras Cir 2013;40:363-9.
https://doi.org/10.1590/S0100-69912013000500003
Osifo DO, Oriaifo IA. Factors affecting the management and outcome of neonatal surgery in Benin City, Nigeria. Eur J Pediatr Surg 2008;18:107-10.
https://doi.org/10.1055/s-2008-1038485
Stey AM, Kenney BD, Moss RL, Hall BL, Berman L, Cohen ME, et al. A risk calculator predicting postoperative adverse events in neonates undergoing major abdominal or thoracic surgery. J Pediatr Surg 2015;50:987-91.
https://doi.org/10.1016/j.jpedsurg.2015.03.023
Ekenze SO, Ajuzieogu OV, Nwomeh BC. Challenges of management and outcome of neonatal surgery in Africa: a systematic review. Pediatr Surg Int 2016;32:291-9.
https://doi.org/10.1007/s00383-016-3861-x
Catania VD, Boscarelli A, Lauriti G, Morini F, Zani A. Risk factors for surgical site infection in neonates: a systematic review of the literature and meta-analysis. Front Pediatr 2019;7:101.
https://doi.org/10.3389/fped.2019.00101
Yamamichi T, Yoshida M, Sakai T, Takayama K, Uga N, Umeda S, et al. Factors associated with neonatal surgical site infection after abdominal surgery. Pediatr Surg Int 2022;38:317-23.
https://doi.org/10.1007/s00383-021-05051-5
Puri A, Lal B, Nangia S. A pilot study on neonatal surgical mortality: a multivariable analysis of predictors of mortality in a resource-limited setting. J Indian Assoc Pediatr Surg 2019;24:36-44.
https://doi.org/10.4103/jiaps.JIAPS_30_18
Bolat F, Kılıç SÇ, Oflaz MB, Gülhan E, Kaya A, Güven AS, et al. The prevalence and outcomes of thrombocytopenia in a neonatal intensive care unit: a three-year report. Pediatr Hematol Oncol 2012;29:710-20.
https://doi.org/10.3109/08880018.2012.725454
Gunnink SF, Vlug R, Fijnvandraat K, van der Bom JG, Stanworth SJ, Lopriore E. Neonatal thrombocytopenia: etiology, management and outcome. Expert Rev Hematol 2014;7:387-95.
https://doi.org/10.1586/17474086.2014.902301
Davenport P, Sola-Visner M. Hemostatic Challenges in Neonates. Front Pediatr 2021;9:627715.
https://doi.org/10.3389/fped.2021.627715
Al Ghadeer HA, Aldhahi RA, Al Dandan FK,Alamer MH, Almulaifi LF, Al Muaibid AF, et al. The prevalence and associated risk factors for neonatal thrombocytopenia among newborns admitted to the neonatal intensive care unit. Cureus 2024;16:e56108.
https://doi.org/10.7759/cureus.56108
Manchanda V, Sarin YK, Ramji S. Prognostic factors determining mortality in surgical neonates. J Neonatal Surg 2012;1:3.
Tamai K, Yorifuji T, Takeuchi A, Fukushima Y, Nakamura M, Matsumoto N, et al. Associations of birth weight for gestational age with child health and neurodevelopment among term infants: a nationwide Japanese population-based study. J Pediatr 2020; 226:135-41.e4.
https://doi.org/10.1016/j.jpeds.2020.06.075
Moreno T, Ehwerhemuepha L, Devin J, Feaster W, Mikhael M. Birth weight and gestational age as modifiers of rehospitalization after neonatal intensive care unit admission. Am J Perinatol 2024;41:e 1668-e1674.
https://doi.org/10.1055/a-2061-0059
Storme L, Boubnova J, Mur S, Pognon L, Sharma D, Aubry E, et al. Review shows that implementing a nationwide protocol for congenital diaphragmatic hernia was a key factor in reducing mortality and morbidity. Acta Paediatr 2018;107:1131-9.
https://doi.org/10.1111/apa.14169
van den Hout L, Schaible T, Cohen-Overbeek TE, Hop W, Siemer J, van de Ven K, et al. Actual outcome in infants with congenital diaphragmatic hernia: the role of a standardized postnatal treatment protocol. Fetal Diagn Ther. 2011;29:55-63.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Chulalongkorn Medical Journal

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.









