Incidence, Risk Factors, and Clinical Outcomes of Multidrug-Resistant Gram-Negative Bloodstream Infection at Banpong Hospital
Keywords:
Multidrug-resistant Gram-negative bacteria, Bloodstream infection, Risk factors, Clinical outcomesAbstract
Background: Multidrug-resistant gram-negative bloodstream infection (MDR GN-BSI) is a critical global health issue associated with limited therapeutic options, increased mortality, and a substantial economic burden. However, data specifically concerning Banpong Hospital remains limited.
Objective: To determine the incidence, risk factors, and clinical outcomes of multidrug-resistant gram-negative bloodstream infection (MDR GN-BSI) at Banpong Hospital, Ratchaburi Province.
Methods: This retrospective analytical study included patients aged 15 years and older with documented gram-negative bloodstream infection between July 1, 2023, and June 30, 2025. Patients were categorized into MDR and non-MDR groups based on international standard definitions. Data were analyzed to determine the incidence, identify associated risk factors, and evaluate the impact on clinical outcomes.
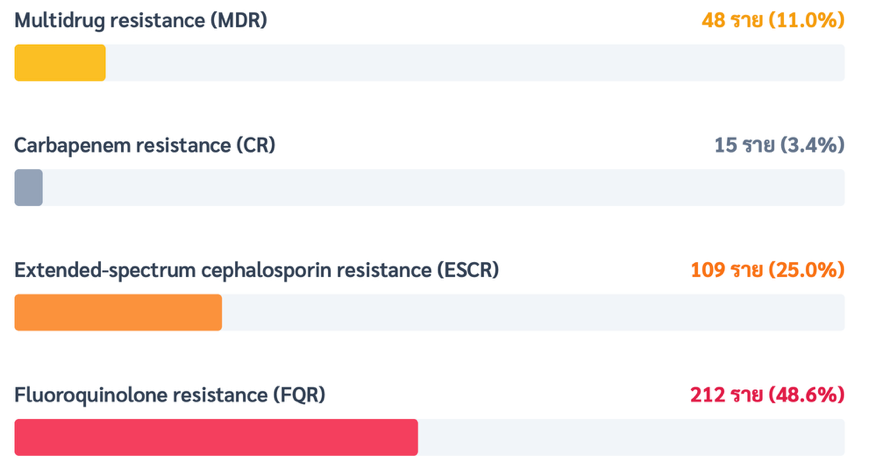
Results: Among 436 patients, the incidence of MDR GN-BSI was 11.0%. The most prevalent pathogens were Escherichia coli and Klebsiella pneumoniae; however, Acinetobacter baumannii exhibited a significantly higher proportion of multidrug resistance (16.7% vs 1.5%, p<0.001). Significant risk factors associated with MDR infection included hospital-acquired infection (adjusted odds ratio [aOR] 4.50, 95% confidence interval [CI] 1.25-16.20, p=0.02), history of fluoroquinolone exposure within the past 90 days (aOR 6.61,95% CI 1.81-24.10, p=0.004) and history of MDR colonization within the past 90 days (aOR 5.92, 95% CI 1.69-20.80, p=0.01). Regarding clinical outcomes, the MDR group had a significantly higher mortality rate compared to the non-MDR group (33.3% vs 7.7%, p<0.001). MDR infection was also associated with an increased risk of septic shock (p=0.04), a longer mean hospital stay by 3.6 days (p=0.01), increased consumption of broad-spectrum antimicrobial agents, and significantly higher mean medical costs (51,502 vs. 31,721 THB per case, p=0.02).
Conclusion: MDR GN-BSI is significantly associated with higher mortality rates and an increased economic burden. Implementation of rigorous infection control and antimicrobial stewardship programs is an immediate priority.
References
World Health Organization. Global antimicrobial resistance and use surveillance system (GLASS) report 2024. Geneva: WHO; 2024.
Logan LK, Weinstein RA. The epidemiology of carbapenem-resistant enterobacteriaceae: the impact and evolution of a global menace. J Infect Dis. 2017;215(Suppl 1):S28–S36. doi: 10.1093/infdis/jiw282.
Tamma PD, Aitken SL, Bonomo RA, Mathers AJ, van Duin D, Clancy CJ. Infectious Diseases Society of America 2022 guidance on the treatment of extended-spectrum β-lactamase producing enterobacterales (ESBL-E), carbapenem-resistant enterobacterales (CRE), and pseudomonas aeruginosa with difficult-to-treat resistance (DTR-P. aeruginosa). Clin Infect Dis. 2022;75(2):187-212. doi: 10.1093/cid/ciac268.
Magiorakos AP, Srinivasan A, Carey RB, Carmeli Y, Falagas ME, Giske CG, et al. Multidrug-resistant, extensively drug-resistant and pandrug-resistant bacteria: an international expert proposal for interim standard definitions for acquired resistance. Clin Microbiol Infect. 2012;18(3):268–81. doi: 10.1111/j.1469-0691.2011.03570.x.
National Antimicrobial Resistance Surveillance Center, Thailand (NARST). Antimicrobial resistance report 2023. Bangkok: NARST; 2024.
Schwaber MJ, Carmeli Y. Mortality and delay in effective therapy associated with extended-spectrum beta-lactamase production in enterobacteriaceae bacteremia: a systematic review and meta-analysis. J Antimicrob Chemother. 2007;60(5):913–20. doi: 10.1093/jac/dkm318.
Sahu C, Jain V, Singh P. Risk factors and outcomes of multidrug-resistant gram-negative infections in intensive care unit patients: a prospective observational study. Indian J Crit Care Med. 2020;24(6):420–6.
Phumart P, Phodha T, Thamlikitkul V, Riewpaiboon A, Prakongsai P, Limwattananon S. Health and economic impacts of antimicrobial resistant infections in Thailand. J Health Syst Res. 2012;6(3):352-60.
Lueangarun S, Thamlikitkul V, Tongsai S. Risk factors and outcomes of carbapenem-resistant enterobacteriaceae bloodstream infection in Thailand. J Med Assoc Thai. 2021;104(7):1010–8.
Apisarnthanarak A, Mundy LM. Epidemiology of multidrug-resistant gram-negative bacteria in Thailand. Infect Control Hosp Epidemiol. 2018;39(9):1180–3.
Soravipukuntorn T, Thammahong A, Charoenpong L, Suttha P, Manosuthi W. Outcomes and associated factors among patients with multidrug-resistant gram-negative bacilli bacteremia at a tertiary care hospital in Thailand. J Med Assoc Thai. 2025;108(1):31-40. doi: 10.35755/jmedassocthai.2025.1.30-41-01303.
Chaisathaphol T, Chayakulkeeree M. Epidemiology of infections caused by multidrug-resistant gram-negative bacteria in adult hospitalized patients at Siriraj Hospital. J Med Assoc Thai. 2014;97(Suppl 3):S35-S45.
Centers for Disease Control and Prevention (CDC). Antibiotic resistance (AR) option protocol. Atlanta (GA): CDC; 2015.
Dalhoff A. Global fluoroquinolone resistance epidemiology and implications for clinical use. Interdiscip Perspect Infect Dis. 2012;2012:976273. doi: 10.1155/2012/976273.
Weiner LM, Webb AK, Limbago B, Dudeck MA, Patel J, Kallen AJ, et al. Antimicrobial-resistant pathogens associated with healthcare-associated infections: summary of data reported to the National Healthcare Safety Network at the CDC, 2011–2014. Infect Control Hosp Epidemiol. 2016;37(11):1288–301. doi: 10.1017/ice.2016.174.
Rizzo K, Horwich-Scholefield S, Shimano KA. Carbapenem and cephalosporin resistance among Enterobacteriaceae: CDC phenotype definitions applied in clinical surveillance. Open Forum Infect Dis. 2019;6(6):ofz244.
Azerefegne EF, Tasamma AT, Demass TB, Tessema AG, Degu WA. Prevalence of multidrug resistant gram-negative bacteria and associated factors among gram-negative blood culture isolates at Tikur Anbessa Specialized Hospital: a retrospective study. BMC Infect Dis. 2025;25(1):1006. doi: 10.1186/s12879-025-11328-0.
Antimicrobial Resistance Collaborators. Global burden of bacterial antimicrobial resistance in 2019: a systematic analysis. Lancet. 2022;399:629-55. doi: 10.1016/S0140-6736(21)02724-0.
Ponyon J, Kerdsin A, Preeprem T, Ungcharoen R. Risk factors of Infections due to multidrug-resistant gram-negative bacteria in a community hospital in rural Thailand. Trop Med Infect Dis. 2022;7:328. doi: 10.3390/tropicalmed7110328.
Porter KA, Rhodes J, Dejsirilert S, Henchaichon S, Siludjai D, Thamthitiwat S, et al. Acinetobacter bacteraemia in Thailand: evidence for infections outside the hospital setting. Epidemiol Infect. 2014;142(6):1317–27. doi: 10.1017/S0950268813002082.
Inchai J, Liwsrisakun C, Theerakittikul T, Chaiwarith R, Khositsakulchai W, Pothirat C. Risk factors of multidrug-resistant, extensively drug-resistant and pandrug-resistant acinetobacter baumannii ventilator-associated pneumonia in a Medical Intensive Care Unit of University Hospital in Thailand. J Infect Chemother. 2015;21(8):570-4. doi: 10.1016/j.jiac.2015.04.010.
Werarak P, Kiratisin P, Thamlikitkul V. Hospital-acquired pneumonia and ventilator-associated pneumonia in adults at Siriraj Hospital. J Med Assoc Thai. 2010;93 (Suppl 1):S126-S138.
Wangchinda W, Laohasakprasit K, Lerdlamyong K, Thamlikitkul V. Epidemiology of carbapenem-resistant enterobacterales infection and colonization in hospitalized patients at a university hospital in Thailand. Infect Drug Resist. 2022;15:2199–210. doi: 10.2147/IDR.S361013.
Zollner-Schwetz I, Zechner E, Ullrich E, Luxner J, Pux C, Pichler G, Schippinger W, et al. Colonization of long term care facility patients with MDR-Gram-negatives during an acinetobacter baumannii outbreak. Antimicrob Resist Infect Control. 2017;6:49. doi: 10.1186/s13756-017-0209-9.
Yassin A, Huralska M, Pogue JM, Dixit D, Sawyer RG, Kaye KS. State of the management of infections caused by multidrug-resistant gram-negative organisms. Clin Infect Dis. 2023;77(9):e46–e56. doi: 10.1093/cid/ciad499.
Lim C, Hantrakun V, Klaytong P, Rangsiwutisak C, Tangwangvivat R, Phiancharoen C, et al. Higher frequency and mortality rate following antimicrobial-resistant bloodstream infections in tertiary-care hospitals compared with secondary-care hospitals in Thailand. medRxiv [Preprint]. 2023:2023.02.07.23285611. doi: 10.1101/2023.02.07.23285611.
European Centre for Disease Prevention and Control. Carbapenem-resistant enterobacterales: third update. Stockholm: ECDC; 2025.
Phodha T, Riewpaiboon A, Malathum K, Coyte PC. Excess annual economic burdens from nosocomial infections caused by multi-drug resistant bacteria in Thailand. Expert Rev Pharmacoecon Outcomes Res. 2019;19(3):305-12. doi: 10.1080/14737167.2019.1537123.
Rattanaumpawan P, Choorat C, Takonkitsakul K, Tangkoskul T, Seenama C, Thamlikitkul V. A prospective surveillance study for multidrug-resistant bacteria colonization in hospitalized patients at a Thai University Hospital. Antimicrob Resist Infect Control. 2018;7:102. doi: 10.1186/s13756-018-0393-2.
Capsoni N, Bellone P, Aliberti S, Sotgiu G, Pavanello D, Visintin B, et al. Prevalence, risk factors and outcomes of patients coming from the community with sepsis due to multidrug resistant bacteria. Multidiscip Respir Med. 2019;14:23. doi: 10.1186/s40248-019-0185-4.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Ratchabhiwat Medical Journal

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Articles in this journal are copyrighted by the x may be read and used for academic purposes, such as teaching, research, or citation, with proper credit given to the author and the journal.use or modification of the articles is prohibited without permission.
statements expressed in the articles are solely the opinions of the authors.
authors are fully responsible for the content and accuracy of their articles.
other reuse or republication requires permission from the journal."


