Development of a Supportive Care Model for Dependent Elderly through Tripartite Mechanism, Thapayha Subdistrict, Palian District, Trang Province
Keywords:
Dependent Older Adults, Tripartite Collaboration, Primary Health CareAbstract
This research and development study aimed to (1) examine the situation and problems of community-based care for dependent older adults, (2) develop a supportive care guideline for dependent older adults through a tripartite mechanism, and (3) evaluate the outcomes and appropriateness of the developed guideline. The study was conducted in Tha Phaya Subdistrict, Palian District, Trang Province. The research was implemented in three phases. Phase 1 explored the situation and problems of care for dependent older adults using in-depth interviews and focus group discussions with 27 participants. Phase 2 involved the development of the supportive care guideline through a workshop meeting of the tripartite mechanism with 15 participants. Phase 3 consisted of pilot implementation and evaluation of the developed approach with 30 pairs of dependent older adults and their caregivers, along with 10 stakeholders. Outcomes were assessed using the Barthel ADL Index, and quality of life was assessed using the EQ-5D-5L. Data were analyzed using descriptive statistics, paired t-tests, and Wilcoxon signed-rank tests, and content analysis.
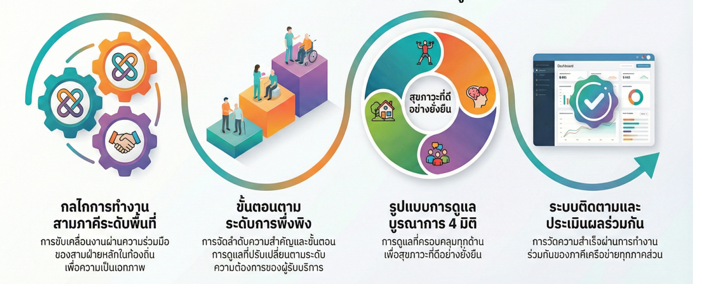
The findings from Phase 1 showed a continuous increase of dependent older adults in the area by experiencing systemic issues, caregiver burden, resource constraints, and a lack of integrated operations. Phase 2, a supportive care guideline for dependent older adults consisted of a tripartite working structure, a four-dimensional integrated care, and a monitoring and evaluation system. Phase 3 found that after implementing the guideline, with increased ADL scores and decreased EQ-5D-5L scores, indicating better quality of life. The developed approach showed high levels of appropriateness and feasibility.
The supportive care guideline for dependent older adults effectively improved both individual outcomes and the community-level care system and can serve as a practical model for scaling up in other areas with similar contexts.
References
กระทรวงสาธารณสุข. (2563). รายงานสถานการณ์ผู้สูงอายุไทย พ.ศ. 2563.
ภาสกร สวนเรือง, อาณัติ วรรณศรี, & สัมฤทธิ์ ศรีธำรงสวัสดิ์. (2561). การพัฒนาระบบการดูแลระยะยาวสำหรับผู้สูงอายุในประเทศไทย. วารสารวิจัยระบบสาธารณสุข, 12(3), 437–451.
สำนักงานสภาพัฒนาการเศรษฐกิจและสังคมแห่งชาติ. (2562). การคาดประมาณประชากรของประเทศไทย พ.ศ. 2553–2583.
สำนักงานหลักประกันสุขภาพแห่งชาติ. (2561). แนวทางการดำเนินงานระบบการดูแลระยะยาวด้านสาธารณสุขสำหรับผู้สูงอายุที่มีภาวะพึ่งพิง.
สำนักงานหลักประกันสุขภาพแห่งชาติ. (2566). คู่มือการดำเนินงานระบบการดูแลระยะยาวด้านสาธารณสุขสำหรับผู้สูงอายุที่มีภาวะพึ่งพิง.
Bandura, A. (1977). Self-efficacy: Toward a unifying theory of behavioral change. Psychological Review, 84(2), 191–215. https://doi.org/10.1037/0033-295X.84.2.191 British
Geriatrics Society. (2019). Comprehensive geriatric assessment. https://www.bgs.org.uk/resources/comprehensive-geriatric-assessment
Hayes, C., et al. (2024). Effectiveness of community-based multidisciplinary integrated care with GP participation: a systematic evaluation. Journal of Multidisciplinary Healthcare, 2024, Article 6437930. https://doi.org/10.1155/2024/6437930
Herdman, M., Gudex, C., Lloyd, A., Janssen, M., Kind, P., Parkin, D., Bonsel, G., & Badia, X. (2011). Development and preliminary testing of the new five-level version of EQ-5D (EQ-5D-5L). Quality of Life Research, 20(10), 1727–1736. https://doi.org/10.1007/s11136-011-9903-x
Kodner, D. L., & Spreeuwenberg, C. (2002). Integrated care: Meaning, logic, applications, and implications—A discussion paper. International Journal of Integrated Care, 2, Article e12. https://doi.org/10.5334/ijic.67
Mahoney, F. I., & Barthel, D. W. (1965). Functional evaluation: The Barthel Index. Maryland State Medical Journal, 14, 61–65.
Polit, D. F., & Beck, C. T. (2006). The content validity index: Are you sure you know what’s being reported? Critique and recommendations. Research in Nursing & Health, 29(5), 489–497. https://doi.org/10.1002/nur.20147
Rogers, E. M. (2003). Diffusion of innovations (5th ed.). Free Press. Uittenbroek, R. J., et al. (2017). Integrated care for older adults improves perceived quality of care: A controlled trial. Journal of General Internal Medicine, 32(6), 630–637. https://doi.org/10.1007/s11606-016-3742-y
United Nations. (2020). World population ageing 2019.
World Health Organization. (2015). World report on ageing and health.
World Health Organization. (2017). Integrated care for older people: Guidelines on community-level interventions.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Journal of Primary Health Research

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.







